Abbie’s Experience of External Cephalic Version (ECV) at 37 Weeks
Being a midwife, particularly one interested in the biomechanics of birth, I was always conscious of my own baby’s position. If you’ve been a receiver of maternity care, you may remember your midwife palpating your abdomen and trying to determine whether the lump they were feeling was a ‘head’ or a ‘bum’, and perhaps you wondered how to tell! You may have also been wondering about the position of your baby’s kicks or the hiccups your baby experienced. I had all this, too, and all signs were pointing towards a breech baby.
I remember attending a growth scan at 32 weeks, and the baby being breech, but telling myself, as I have always told anybody in my care, ‘there’s plenty of time for baby to turn’, which is true! But I was doubting it myself.
At 36 weeks, as per my trust’s policy, when my midwife palpated the baby as being in the breech position, I was offered a presentation scan. I went in early, and my midwife was right- the baby was breech! At this point, he had been breech or transverse lie for around ten weeks. The sonographer determined he was in a frank breech position. With my midwife knowledge, I knew this was a position that was not contraindicated for an ECV, so as per trust guidance, I was offered a discussion with a consultant who offered me no action (go into labour), an elective caesarean at 39 weeks or an ECV. I was talked through the evidence and the risks and benefits B. R. A. I. N. I had already decided on an ECV, and the consultant was happy to try it. At this point, I was 37 weeks.
As my husband was at work, I was quite nervous, but I knew the professionals caring for me, so I felt comforted by that. But it was interesting being on the ‘receiving’ end, considering I had supported families through ECV many times. I was advised to have a CTG to ensure my baby was well, which was interesting as I had not had one beforehand. I also had a full set of observations. Once the professionals were happy that the CTG showed the baby was displaying good signs of well-being. I was given terbutaline, a muscle relaxant, and told it might make my heart feel it was racing- it did!
Holding a midwife’s hand, the consultant began trying to turn the baby. The initial jab of identifying the baby’s bum in the pelvis was a little uncomfortable, but then once the baby got to 180 degrees, he flipped to cephalic (head down!). We were all very relieved. I was then advised to go back onto the CTG to ensure the baby was well following this and monitored for a period of time. Eventually, the heart racing of the terbutaline wore off, and my husband was relieved all was well. I was disconnected from the CTG and given a time and date to return the following week to ensure the baby was still cephalic.
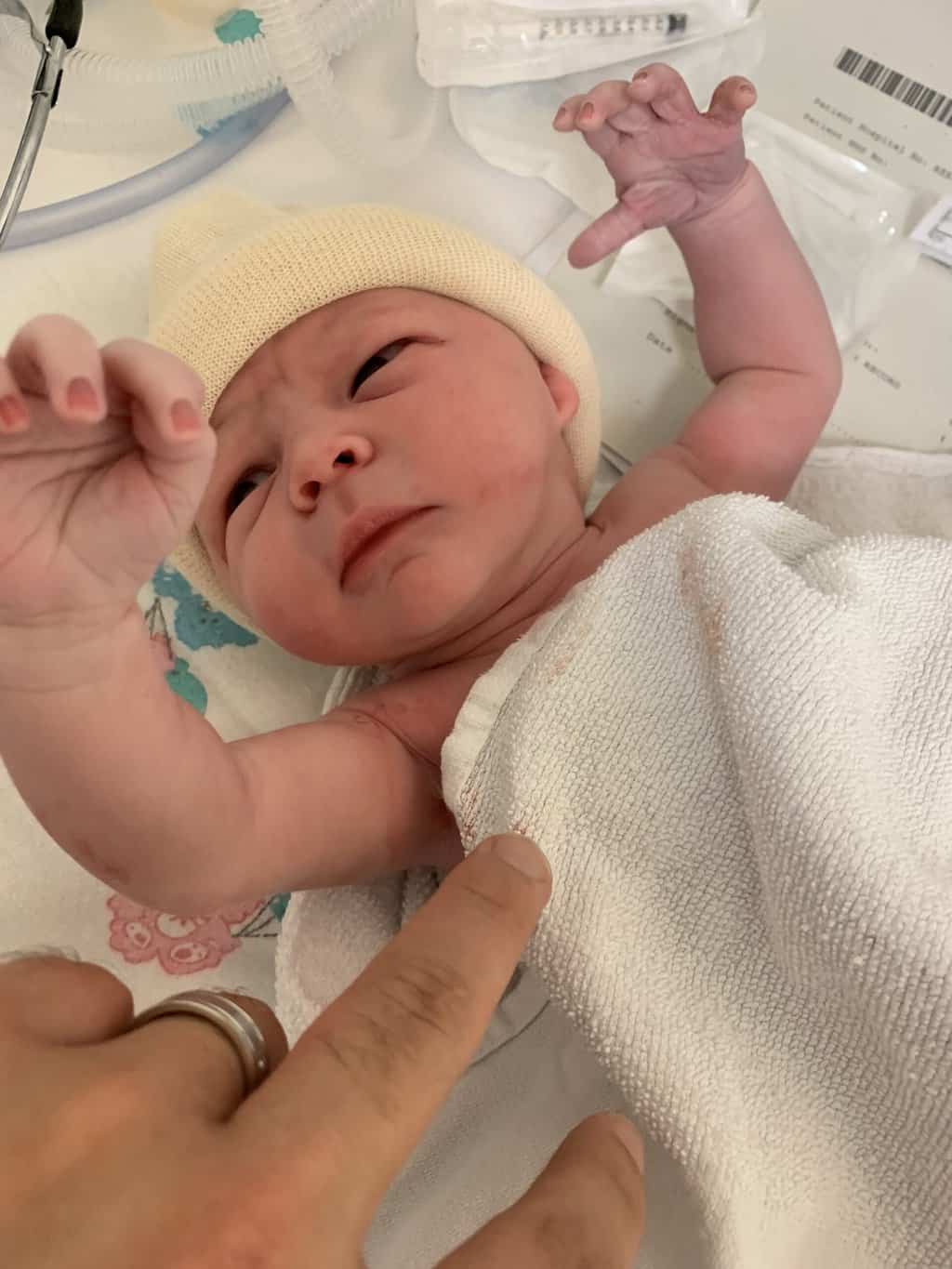
A week later, the baby remained cephalic and at 40+3, I spontaneously went into labour and birthed a cephalic baby with a lovely round head (very typical, given that he was breech for so long!).