Factsheet – Lotus Birth
Ali Monaghan
Independent Midwife
Twitter @alithemidwife Instagram @alimonaghan
Summary
What we know
Lotus birth, or the practice of umbilical cord non-severance, involves keeping the umbilical cord intact and connected to the baby until it naturally detaches on its own, usually between postnatal day 3-10.1 This practice was first described (and named after) Clair Lotus Day in 1974, who observed the phenomenon of an uncut cord in chimpanzees and then went on to request a lotus birth for her own upcoming hospital birth.2,3 Afterwards, lotus birth was spread by midwife and yoga practitioner Jeannine Parvarti Baker in the United States, and by Shivam Rachana, founder of the International College of Spiritual Midwifery, and Dr. Sarah Buckley in Australia. While the overall incidence of lotus birth is unknown, the practice has been observed in many countries, including the US, Australia, the United Kingdom, Italy and Turkey.4
Proponents of lotus birth cite the many benefits offered by this practice. The advantages to delayed cord clamping (DCC) have been well documented in the medical literature.5,6 At the time of birth, one third of the fetal blood volume is contained in placental circulation. Allowing for DCC of at least a minute, and better yet, optimal cord clamping (OCC), which involves waiting until the cord has stopped pulsing and turned white, leads to improved neonatal oxygenation levels during extrauterine transition, improved newborn haematocrit and haemoglobin levels, increased ferritin and decreased anaemia rates during infancy, and decreased risks of intraventricular haemorrhage and the need for blood transfusions in preterm babies.7,8 A lotus birth ensures that all of these benefits occur.
However, in qualitative research, women who have chosen lotus births cite many additional benefits to the practice, such as an opportunity for undisturbed bonding with their babies, a preservation of the naturalness of birth, and a spiritual regard for the placenta as an integral part of their baby, something which must be honoured and respected.4 A Lotus Birth helps preserve the mother-infant bond and helps to enforce a “lying-in” period, or a “breaking forth”, as Dr. Sarah Buckley terms it.3 A baby who is still attached to the cord is a visual reminder to visitors that the baby is still new and needs to be protected, and also helps to prevent the baby from being passed from one excited relative to the next (potentially to the mum and baby’s detriment). Additionally, because babies are slightly more difficult to dress with an intact cord, holding the baby skin-to-skin comes more naturally, which in turn can help to establish breastfeeding in the early postnatal days.9



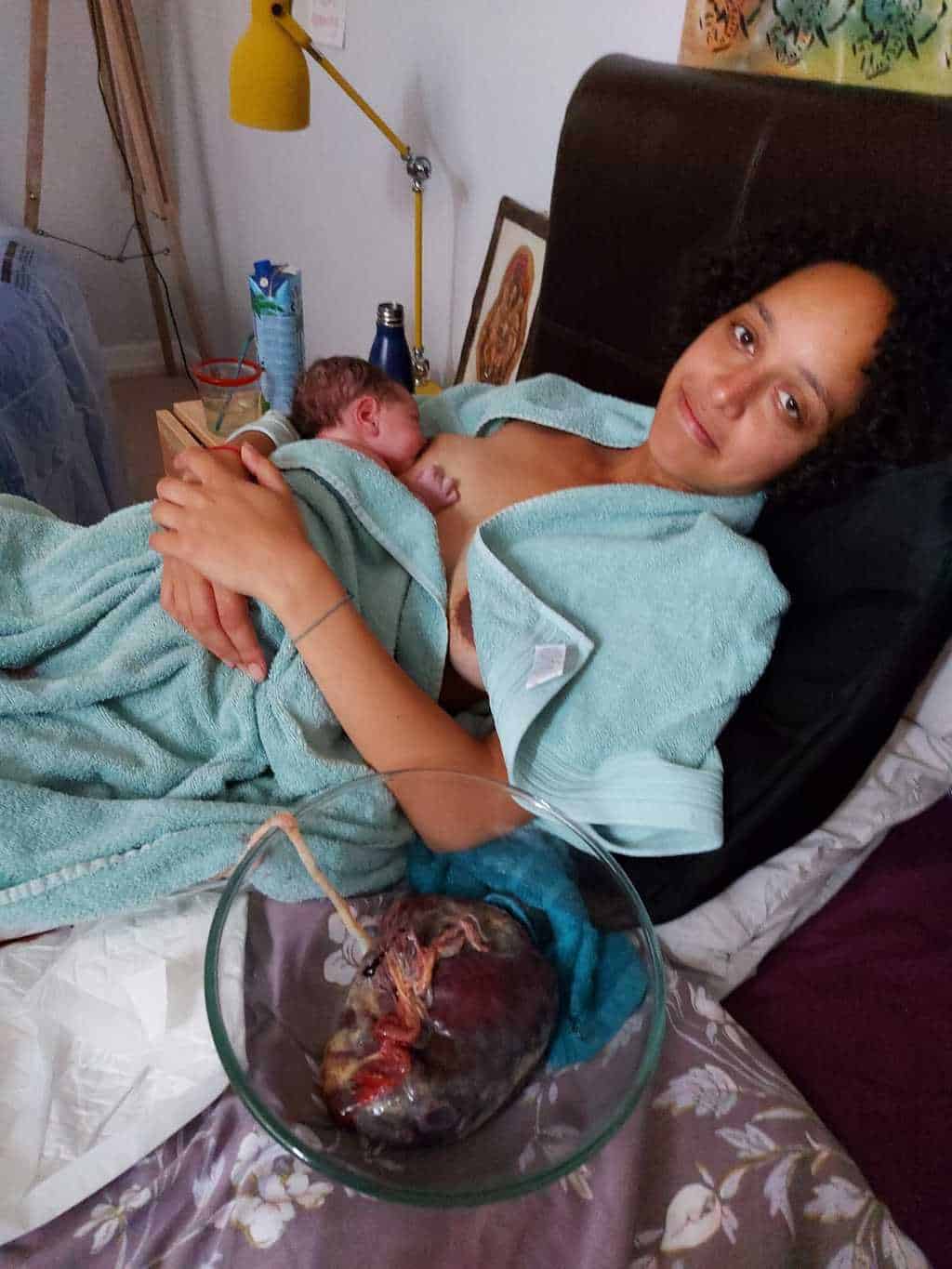
Photographs – Cat Hess @cat.thedoula
What we don’t know
Unfortunately, the medical literature is limited to case-reports and some qualitative studies about people’s beliefs and experiences with lotus birth, as well as explorations of different cultural rituals, practices and traditions surrounding the placenta.10 There are no high-quality quantitative studies available on this topic to advise on the safety of this practice. However, some case reports have indicated that lotus birth can pose a risk for infection, sepsis, jaundice and idiopathic neonatal hepatitis.11,12 In the past, the Royal College of Obstetricians and Gynaecologists has issued a statement advising women about the lack of robust evidence on this topic, although the RCOG statement has now been archived and is no longer available online. Should a family decide to proceed with a lotus birth, signs of infection should be taught to family members, and any signs of infection should be responded to promptly.
Mothers and families: how to use the evidence
While lotus birth is a rare practice, it is a valid choice and should be supported by midwives and maternity health care providers within the framework of facilitating and respecting women and birthing people’s birth choices.13 If a lotus birth appeals to you, it would be good to speak with your midwife about your desire prior to giving birth, and to include this practice in your birth plan. Resources are listed below which my help to guide your decision and assist with planning for the postnatal period. The steps below serve as a general guide on how to carry out a lotus birth:
1. The newborn is kept skin-to-skin on the birthing person’s chest after birth while the placenta is spontaneously delivered.
2. The umbilical cord is not clamped. After a period of 5 minutes, blood flow between the placenta and baby has usually ceased, as demonstrated by the absence of a pulse felt in the cord and the cord turning white.
3. The placenta is examined by the midwife or health care provider to determine that it is intact.
4. The placenta is then washed with warm water and dried, and then drained in a sieve or colander for 24 hours.
5. An absorbent gauze compress or dry nappy can then be placed underneath the placenta to absorb any excess blood or liquid, and should also be changed daily to prevent the growth bacteria.
6. Alternatively, a mixture of 1 kg salt and 0.5 kg rosemary and/or 0.5 kg dried lavender can be prepared, and the placenta can be laid on a bed of this salt, and liberally sprinkled with salt. This is done to help dry out the placenta, prevent infection and eliminate foul odour. The salt should also be changed daily.
7. The placenta can be stored in a lightweight, breathable bag which allows for air circulation until the cord separates from the newborn.
8. The umbilical cord will become dry and hard after one day.
9. The newborn, cord and placenta are then carried together until the umbilical cord separates from the newborn spontaneously, at which point the placenta can be buried, stored or dried etc.4,14
Midwives and birth workers: how to use the evidence
While lotus birth is a very rare request, it’s important to be aware of both its benefits and potential risks in order to facilitate informed consent discussions about lotus birth and to be able to answer questions around the practice. In the antenatal period, it’s helpful to be able to signpost women to good sources of information on lotus birth. In the immediate postnatal period, a midwife or birthworker may be asked to assist with placental preparation, and it’s valuable to be aware of this process if requested. Some providers may also find it helpful to prepare written information on signs and symptoms of infection, which can be given to parents in addition to verbal instructions. In all cases, parents should be made aware of potential infection signs in their newborn, including erythema or warmth around the umbilical cord, foul-smelling exudate/ discharge from the cord, temperature fluctuations (either a raised temperature or inability to maintain normal temperature), worsening jaundice, or a baby who is becoming increasingly sleepy and difficult to rouse, and should be instructed to seek prompt medical attention if these signs arise.
Links to other resources
 Books
Books
Lotus Birth book by Shivam Rachana: https://www.lotusbirth.net/
 Websites
Websites
Dr. Sarah Buckley: http://www.sarahbuckley.com/
 Videos
Videos
Lotus Birth DVD for education purposes: https://birthinternational.com/product/lotus-birth-dvd/
References
1 Buckley, S. Lotus Birth: a ritual for our times. Midwifery Today. 2003; 67: 36-38.
2 Zinsser, LA. Lotus birth, a holistic approach on physiological cord clamping. Women and Birth. 2018; 31: e73-e76.
3 Buckley, S. Gentle Birth, Gentle Mothering. Berkeley, CA: Celestial Arts; 2009.
4 Gönenç, IM, Aker, MN and Ay, E. Qualitative Study on the Experience of Lotus Birth. Journal of Obstetric, Gynecologic & Neonatal Nursing (JOGNN). 2019; 48: 645-653.
5 Eichenbaum-Pikser, G, Zasloff, JS. Delayed Clamping of the Umbilical Cord: A Review with Implications for Practice. Journal of Midwifery and Women’s Health. 2009; 54: 321-326.
6 Raju, TNK, Singal, N. Optimal Timing for Clamping the Umbilical Cord After Birth. Clinical Perinataology. 2012; 39(4): 889-900. doi 10.1016/j.clp.2012.09.006
7 National Institute of Health and Care Excellence (NICE). Intrapartum Care, Quality Statement 6: Delayed Cord Clamping. https://www.nice.org.uk/guidance/qs105/chapter/Quality-statement-6-Delayed-cord-clamping Published 2015. Accessed 8th June 2020.
8 Royal College of Obstetricians and Gynaecologists (RCOG). Clamping of the Umbilical Cord and Placental Transfusion; Scientific Impact Paper No. 14. https://www.rcog.org.uk/globalassets/documents/guidelines/scientific-impact-papers/sip-14.pdf Puublished 2015. Accessed 30th October 2020.
9 Lim. R. Lotus Birth: Asking the Next Question. Midwifery Today. 2001; 58(summer 2001): 14-16.
10 Burns, E. More than Clinical Waste? Placenta Rituals Among Australian Home-Birthing Women. The Journal of Perinatal Eduation. 2014; 23(1): 41-49.
11 Ittleman, BR, German, KR, Scott, E, Walker, V, Flaherman, VJ, Szabo, J and Beavers, JB. Umbilical Cord Nonseverance and Adverse Neonatal Outcomes. Clinical Pediatrics. 2019; 58(2): 238-240.
12 Tricarico, A, Bianco, V, Di Biase, AR, Iughetti, L, Ferrari, F and Berardi, A. Lotus Birth Associated with Idiopathic Neonatal Hepatitis. Pediatrics and Neonatology. 2017; 58(3): P281-282.
13 National Maternity Review. Better Births: Improving Outcomes of Maternity Services in England. https://www.england.nhs.uk/wp-content/uploads/2016/02/national-maternity-review-report.pdf Published 2016. Accessed 9th June 2020.
14 Rachana, S. Lotus Birth: Leaving the Umbilical Cord Intact. https://www.lotusbirth.net/ Published 2013. Accessed: 30 October, 2020.